
Главная страница Случайная страница
КАТЕГОРИИ:
АвтомобилиАстрономияБиологияГеографияДом и садДругие языкиДругоеИнформатикаИсторияКультураЛитератураЛогикаМатематикаМедицинаМеталлургияМеханикаОбразованиеОхрана трудаПедагогикаПолитикаПравоПсихологияРелигияРиторикаСоциологияСпортСтроительствоТехнологияТуризмФизикаФилософияФинансыХимияЧерчениеЭкологияЭкономикаЭлектроника
Special Pathology. Diseases of the cardiovascular system stand among the first in the list of diseases of internal organs
|
|
Diseases of the cardiovascular system stand among the first in the list of diseases of internal organs. They are a frequent cause of early disability and untimely death of patients. Most common are ischaemic heart disease, rheumatism and rheumatic heart diseases, endocarditis, myocarditis of various genesis, and essential hypertension.
Special Part
Chapter 6. Blood Circulatory System
 Rheumatism
Rheumatism
Rheumatism is a general infectious and allergic disease in which connective tissues, mainly of the cardiovascular system, are affected by inflammation; joints, serous membranes, internal organs, and the central nervous system are often involved. Rheumatism is a collagenous disease, i.e. a disease characterized by a systemic and progressive derangement of connective tissue.
Rheumatism was classified as an independent disease with typical affections not only of the joints but mainly of the heart in 1835 by a French clinicist Bouillaud and in 1836 by the Russian physician Sokolsky. Until that time rheumatism had been considered a disease of joints.
Aetiology and pathogenesis. Beta-haemolytic streptococcus of group A is believed to be the causative agent of rheumatism. This conjecture is confirmed by (1) frequent incidence of rheumatism following streptococcal infection; (2) increased antibody titres to various antigens and enzymes of the streptococcus in the blood of rheumatic patients; (3) successful prophylaxis of rheumatism by antibacterial preparations.
The pathogenesis of rheumatism is complicated and not well studied. At the present time, the development of the disease is described as follows. Most persons affected by streptococcus develop stable immunity. This immunity does not develop in 2-3 per cent of the affected subjects due to weakness of their defence mechanisms and they become sensitized by the streptococcus antigen. In these conditions the infection re-enters the body to cause a hyperergic response in connective tissues; clinical signs of the disease thus develop. Autoimmune processes are very important in the onset of rheumatism. The affected connective tissue acquires antigenic properties; auto-antigens (secondary antigens) cause formation of aggressive auto-antibodies. They affect not only the connective tissue that has already been affected by the primary antigen but also intact tissue to aggravate the pathology. Re-infection, cooling, and overstrain promote formation of new auto-antigens and auto-antibodies to strengthen the pathological reaction of the upset immunity and to provide conditions for the recurring progressive course of the disease.
Pathological anatomy. Four phases of derangement of connective tissue are differentiated in rheumatism: (1) mucoid swelling; (2) fibrinoid changes; (3) granulomatosis; and (4) sclerosis.
Mucoid swelling is characterized by superficial derangement of connective tissue which involves mainly the interstitial substances and only insignificantly the collagenous complex. The processes occurring at this stage are reversible. Derangement of connective tissue occurring at the fibrinoid stage is deep and irreversible. Histiocytes form granulomas (Aschoff-Talalaev granulomas, rheumatic nodules) which contain lymphoid cells, leucocytes, and car-diohistiocytes. Rheumatic granulomas would be usually located in perivascular connective tissue of the myocardium, in the endocardium, and (in slightly modified form) in synovial
membrane of the articular bursa, periarticular and peritonsillar tissue, vascular adventitia, etc. At the phase of sclerosis, a cicatrix is gradually formed, which may develop at the site of fibrinoid changes and also as a result of cicatrization of rheumatic granulomas. Each phase of rheumatism lasts on the average one or two months, and the entire cycle continues for at least six months.
Tissues in the zone of old cicatrices may be affected in relapses of rheumatism and sclerosis may develop. Affection of connective tissue of the valvular endocardium which causes sclerosis and deformation of the valve cusps (their adhesion to one another) is the most common cause of heart diseases, while relapses of rheumatism (recurring attacks) aggravate affections of the valves. Non-specific exudative reactions may develop, mostly in the pericardium and the joints, and less frequently in the pleura, peritoneum, and the myocardium. Vasculitis (capillaritis, arteritis, phlebitis) are also non-specific rheumatic affections.
Clinical picture. The clinical picture of rheumatism is quite varied and depends mostly on the localization of the inflammatory changes in connective tissues of various organs and on acuity of the rheumatic process. As a rule, the disease develops in 1—2 weeks after a streptococcal infection (e.g. tonsillitis, pharyngitis or scarlet fever). Most patients develop subfebrile temperature, weakness, and hidrosis. Later (in 1—3 weeks), new symptoms develop to indicate affection of the heart. The patient complains of palpitation and intermissions in the work of the heart, the feeling of heaviness or pain in the heart, and dyspnoea.
Less frequently the onset of the disease is acute. Remitting temperature develops (38—39 °C), which is accompanied by general asthenia, fatigue, and perspiration. Simultaneously (or several days later) the patient feels pain in the joints (mostly in large joints, such as the ankle, knee, shoulder, elbow joints, and in hands and feet). Affections of the joints are usually multiple and symmetric. The migrating character of pain is also characteristic: pain disappears in one joint and develops in others. Rheumatic polyarthritis is usually benign. Acute inflammation subsides in a few days, although dull pain in the joints may persist for a long time. Abatement of inflammation in the joints does not mean recovery because other organs become involved in the pathological process. The cardiovascular system is mostly involved, but the skin, serous membranes, lungs, liver, kidneys, and the nervous system may also be affected.
Examination of the patient with active rheumatism reveals pallid skin (even at elevated temperature) and increased perspiration. In some patients, the skin of the chest, neck, abdomen, and the face is affected by annular erythema (pale-pink painless rings not elevating over the surrounding skin). In other cases nodular erythema develops: circumscribed indurated dark red foci on the skin varying in size from a pea to a plum; they are usually found on the lower limbs. If permeability of capillaries is increased, small haemorrhages into the skin sometimes occur. In rare cases, rheumatic subcutaneous nodules (firm, painless formations varying in size
Special Part
Chapter 6. Blood Circulatory System
 | |||
 | |||
 from a millet grain to a bean) can be palpated, mostly on the extensor surfaces of the joints, along the course of tendons, and in the occipital region. The involved joints are swollen and oedematous, the overlying skin reddens and becomes hot to the touch. Articulation becomes very limited.
from a millet grain to a bean) can be palpated, mostly on the extensor surfaces of the joints, along the course of tendons, and in the occipital region. The involved joints are swollen and oedematous, the overlying skin reddens and becomes hot to the touch. Articulation becomes very limited.
Lungs are affected in very rare cases. This is specific rheumatic pneumonia. Dry pleurisy or pleurisy with effusion are more common. Heart affections may be the only clinical manifestation of rheumatism. On the other hand, practically all rheumatic patients have their heart muscle affected (rheumatic myocarditis). Rheumatic myocarditis is characterized by dyspnoea, the feeling of heaviness and pain in the heart, palpitation, and intermissions in the heart work. In addition, certain objective signs are found: enlargement of the heart, decreased heart sounds (especially the first sound); gallop rhythms develop in severe affection of the myocardium. A soft systolic murmur can be heard at the heart apex. It is associated with relative incompetence of the valve or affection of the papillary muscles. The pulse is small and soft; tachycardia and arrhythmia are frequent. Arterial pressure is usually decreased. Circulatory insufficiency rapidly develops in grave diffuse myocarditis. Myocardial car-diosclerosis develops in benign outcome of the disease.
Rheumatic myocarditis usually concurs with rheumatic endocarditis (rheumocarditis). Early endocarditis signs are not pronounced (symptoms of myocarditis prevail). Further development of the heart disease proves the presence of endocarditis. At earlier stages of endocarditis systolic murmurs are coarser than in myocarditis; the murmur becomes louder after exercise; in some cases it becomes " musical". Diastolic murmur may be heard as well. It is probably explained by deposition of thrombotic mass on the valve cusps which produces turbulence in the blood flow as it passes from the atrium to the ventricle. These thrombotic deposits on the valves can leave their seat and become the cause of embolism or infarctions in various organs (e.g. the kidneys or the spleen). The mitral valve is mostly affected in endocarditis. Next in incidence follows the aortkTvalve; the tricuspid valve Isaffected still less frequently. If early attacks of rheumatic endocarditis are treated timely, development of the valvular heart disease may be prevented.
In a grave course of rheumatism the affection of the myocardium and endocardium may combine with rheumatic pericarditis, i.e. all membranes of the heart may be involved (pancarditis). Pericarditis may be dry or exudative.
The alimentary system is rarely affected. Acute pain in the abdomen (the abdominal syndrome) associated with rheumatic peritonitis (mostly in children) sometimes occurs. The liver is affected in certain cases (rheumatic hepatitis).
Affections of the kidneys are also common. Protein or red blood cells can be found in the urine due to affections of the renal vessels and (less frequently) developing nephritis.
The nervous system is often involved in rheumatism. This is due to either rheumatic vasculitis (attended by small haemorrhages or thrombosis of cerebral vessels) or inflammation of the brain and the spinal cord. Children would develop encephalitis with predominant localization in the subcortical nodes (chorea minor). It is manifested by emotional lability and hyperkinesia (abnormal movements of the extremities, the trunk, and the facial muscles).
Special laboratory tests help diagnose rheumatism. Moderate leucocytosis (with a shift to the left) is characteristic of acute rheumatism; eosinophilia, mono- and lymphocytosis may further develop. The erythrocyte sedimentation rate is always increased (to 50-70 mm/h in grave cases). Dysproteinaemia is characteristic: the albumin content drops below 50 per cent, the globulin content increases, and the albumin-globulin factor decreases below unity. A proteinogram shows increased a2-globulin and 7-globulin fractions; fibrinogen content increases to 0.6-1 per cent (normally it does not exceed 0.4 per cent). The blood contains C-reactive protein which is absent in healthy individuals. The level of mucoproteins increases and it can be revealed by a diphenylamine test. The titres of an-tistreptolysine O, antistreptohyaluronidase, and antistreptokinase increase significantly.
ECG often shows deranged conduction, especially atrioventricular block of the first and second degree, extrasystole or other rhythm disorders, and decreased voltage of the ECG waves. Defective nutrition of the myocardium due to its inflammation can change the T wave and lower the S-T segment. Phonocardiograms show specific rheumocarditic changes in heart sounds, the appearance of murmurs, etc.
Course. An active rheumatic process continues for three to six months; in some cases it may be longer. Depending on the strength of the clinical symptoms and the character of the disease course, three degrees of rheumatic activity are distinguished: (1) maximum active (acute) process with continuous relapses; (2) moderately active or subacute; and (3) rheumatism with minimal activity (flaccid or latent). If the clinical symptoms of the disease are absent and no signs of active rheumatism are revealed by laboratory testing, rheumatism is considered inactive.
| 19-1556 |
Rheumatism is characterized by relapses (recurring attacks) which are provoked by infection, overcooling, and physical overstrain. The clinical symptoms of relapses resemble the primary attack of the disease, but the signs of affection of the joints or serous membranes are less pronounced. Symptoms of heart affection prevail.
Special Part ''
Chapter 6. Blood Circulatory System
 Treatment. Active rheumatism is treated at hospital. The patient should stay in bed and be given desensitizing and anti-inflammatory preparations, corticosteroid hormones, acetylsalicylic acid, amidopyrin, butadion, and chloroquine. Antibiotics are given as well, especially in the presence of infectious foci (e.g. carious teeth, tonsillitis or sinusitis). These foci should be eliminated by appropriate means.
Treatment. Active rheumatism is treated at hospital. The patient should stay in bed and be given desensitizing and anti-inflammatory preparations, corticosteroid hormones, acetylsalicylic acid, amidopyrin, butadion, and chloroquine. Antibiotics are given as well, especially in the presence of infectious foci (e.g. carious teeth, tonsillitis or sinusitis). These foci should be eliminated by appropriate means.
Prophylactic measures against rheumatism include hardening of the body, improvement of housing and working conditions, and control of streptococcus infection (treatment of chronic tonsillitis, otitis, sinusitis, etc.). Rheumatic patients should be kept under regular medical observation. To prevent relapses of rheumatism in spring and autumn, medicamentous prophylaxis should be given (bicillin in combination with salicylates or amidopyrine and chloroquine).
Bacterial (Septic) Endocarditis
Bacterial endocarditis is a severe general disease characterized by inflammation of the endocardium and ulceration of the heart valves in the presence of sepsis.
Acute bacterial endocarditis (a manifestation of acute sepsis) and subacute bacterial endocarditis are distinguished according to the course of the disease.
SUBACUTE BACTERIAL ENDOCARDITIS
Aetiology and pathogenesis. Subacute bacterial endocarditis (endocarditis septica lenta) is usually caused by Streptococcus viridans, less frequently by enterococcus and Staphylococcus albus or St. aureus. In most cases, protracted bacterial endocarditis affects the valves that are changed by the rheumatic process, or develops in congenital heart diseases. It is believed that upset haemodynamics in heart diseases inflicts microinjuries to the valves which provoke changes in the endocardium, especially along the contact line of valve cusps. Factors weakening immunological reactions facilitate the development of the disease.
Pathological anatomy. This is characterized by the presence of ulcerous endocarditis. Ulcerated surfaces become covered with polyp-like thrombotic mass which sometimes looks like cauliflower. The valves become sclerosed and disfigured. The aortic valve is especially frequently involved. Endothelium of fine vessels is affected to cause vasculitis or throm-bovasculitis: vascular permeability increases and small haemorrhages develop in the skin and mucosa.
Clinical picture. The symptoms of the disease mainly depend on toxaemia and bacteriaemia. The patients complain of weakness, rapid fatigue,
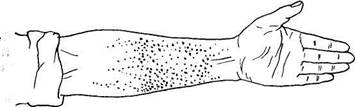
and dyspnoea. As a rule, subfebrile fever first develops, which is followed by irregular elevation of temperature to 39 °C and more. Chills and excess sweating are characteristic. The skin and visible mucosa are pallid due to anaemia and aortic incompetence, which is characteristic of this disease. The skin sometimes becomes yellowish-grey (coffee with milk). Small haemorrhages in the skin, mucosa of the mouth (especially the soft and hard palate), on conjunctiva, and the eyelid folds (the Libman-Lukin symptom) indicate affection of the joints. Positive Konchalovsky-Rumpel-Leede sign is another indication of this process: if the arm of the patient is compressed by a tourniquet or by a cuff of a Riva-Rocci sphygmoma-nometer, multiple petechiae appear on the flexor surface of the elbow, and also distally of it (Fig. 68). Brittleness of capillaries can also be established by pinching the skin. In most cases the patient's fingers become clubbed (Hippocratic fingers), while the nails are flat like a watch glass.
Auscultation of the heart reveals signs of acquired or congenital diseases in most patients. Development of endocarditis is attended by the appearance of functional murmurs due to anaemia and murmurs that are caused by changes in the affected valve. Aortic valve cusps are usually involved, and signs of aortic incompetence therefore develop, while symptoms of mitral insufficiency develop in affections of the mitral valve.
|
| Fig. 68. Konchalovsky-Rumpel-Leede symptom. |
Subacute bacterial endocarditis is characterized by embolisms (caused by decomposing thrombotic deposits on the valves) in the vessels of the spleen, kidneys or brain, followed by infarction of the involved organ. The spleen is enlarged due to the response of the mesenchyma to sepsis. The •disease is characterized by involvement of the kidneys which gives the picture of diffuse glomerulonephritis and much less frequently focal glomerulonephritis without pronounced symptoms (slight proteinuria and haematuria, and insignificant cylindruria). Hypochromic anaemia (caused by increased haemolysis and inhibited erythropoiesis) and a markedly increased ESR are also characteristic. Leukocyte count varies. Eosinophil count decreases and there is a tendency to monocytosis and histiocytosis. If the number of histiocytes in blood taken from the ear lobe after its massage increases compared with their amount in the blood taken before the
19*
Special Part
Chapter 6. Blood Circulatory System

 massage (Bittorf-Tushinsky test), it indicates affection of the vascular en-dothelium. Biochemical study of the blood reveals dysproteinaemia (hypoalbuminaemia, increased content of gamma-globulins); thymol and formol tests are positive. The causative agent of the disease can be revealed in blood cultures.
massage (Bittorf-Tushinsky test), it indicates affection of the vascular en-dothelium. Biochemical study of the blood reveals dysproteinaemia (hypoalbuminaemia, increased content of gamma-globulins); thymol and formol tests are positive. The causative agent of the disease can be revealed in blood cultures.